- Published on
Release of New York External Appeal Dashboard
- Authors

- Name
- Mike Gartner, PhD
Introduction
Today, we're releasing a new dashboard that makes New York's external appeal data more accessible and usable for patients, advocates, policymakers, and researchers.
You can learn more and try it out at https://appeal-explorer.persius.org.
New York has long been a leader in providing comprehensive access to data that illuminates the extent, harm, and inequitable nature of wrongful coverage denials. Their external appeal database documents Independent Medical Reviews across different types of health insurance in the state. It's a rich, informative dataset that's surprisingly underutilized in popular media and by advocates, patients, regulators, and policymakers seeking to understand patterns of wrongful denials.

Figure 1. A screenshot of our interactive dashboard exploring New York's external appeal data.
Why External Appeals Matter
External appeals, or independent medical reviews, are appeals reviewed by independent third parties. They contrast sharply with internal appeals, which patients must typically exhaust first, and which involve review of denials by the same entity that made the initial denial. While independent medical reviewers have their own biases, they lack the plain financial incentive at play in internal reviews: the reviewer's employer has no financial interest in preferring one outcome over the other.
For this reason, external appeal outcomes are an imperfect but important proxy for the prevalence and distribution of wrongful denials. External appeal overturns reflect denials that were typically both inappropriate and inappropriately decided during first-level appeals. High rates of external appeal overturn, especially when inequitably distributed, are troubling signs that wrongful denials are being administered for some patient populations at inappropriately high rates.
The Data
New York's external appeal database consists of individual appeal cases. Each case includes metadata about the situation (type of health insurance, specific insurer, appeal outcome, broad category of diagnosis and treatment) and plain text summaries from reviewing physicians. Combined, these fields provide a rich mechanism for understanding the circumstances surrounding individual denials, subsequent internal appeals, and the medical necessity as determined by third-party reviewers.
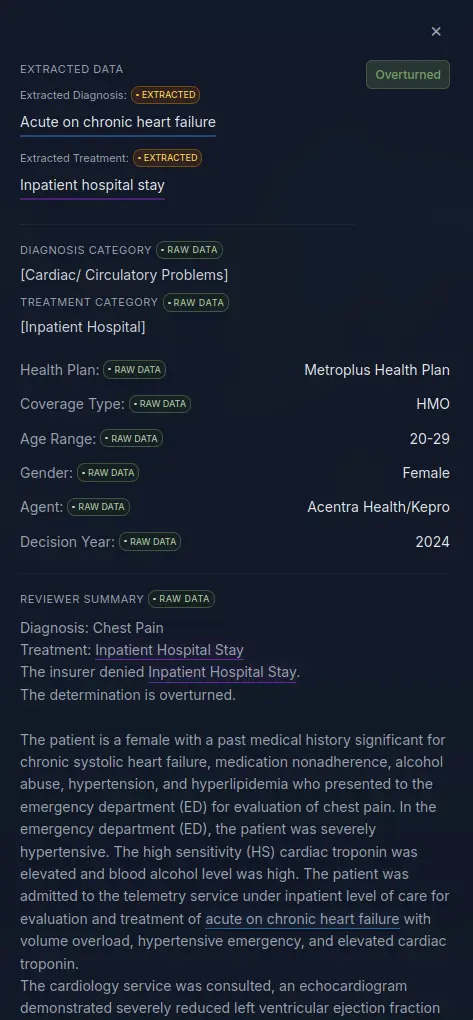
Figure 2. A screenshot showing the contents of a single appeal case in the database, as viewed from our dashboard.
Dashboard Features
Our dashboard serves as a user interface for the raw data that's complementary to what the Department of Financial Services provides in their officially hosted version. As heavy users of this database for years, we've learned there are many features we want in a UI for this data that don't currently exist. The features most important to us, and which we're releasing with this first beta, are:
1. Quick Inspection of Appeal Overturn Rates
We want the ability to quickly inspect appeal overturn rates stratified by any of the metadata fields. This is only possible via a hacky workaround in the DFS maintained dashboard.
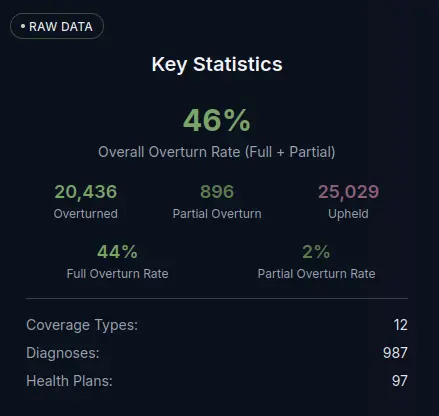

Figure 3. A screenshot showing the approach in our dashboard to supporting quick inspection of appeal overturn rates stratified by filter sets.
2. Filtering by Specific Diagnoses and Services
We want the ability to filter cases by the specific diagnoses and services in question. This feature isn't supported in the DFS dashboard, and is actually complicated to support technically. While diagnoses and services at question in each appeal are typically contained in the review summaries, they can't merely be verified by search or matching, because summaries often also include past histories with references to diagnoses and services that are not the diagnoses and services in question.
This feature is nonetheless critical for our interest in shining a light on the inequitable nature of wrongful denials, and illustrating the harm on vulnerable populations. For example, Figure 4 shows that external appeal cases involving services for Diabetic Ketoacidosis (a serious, potentially life-threatening complication) are overturned on external appeal at staggering rates.
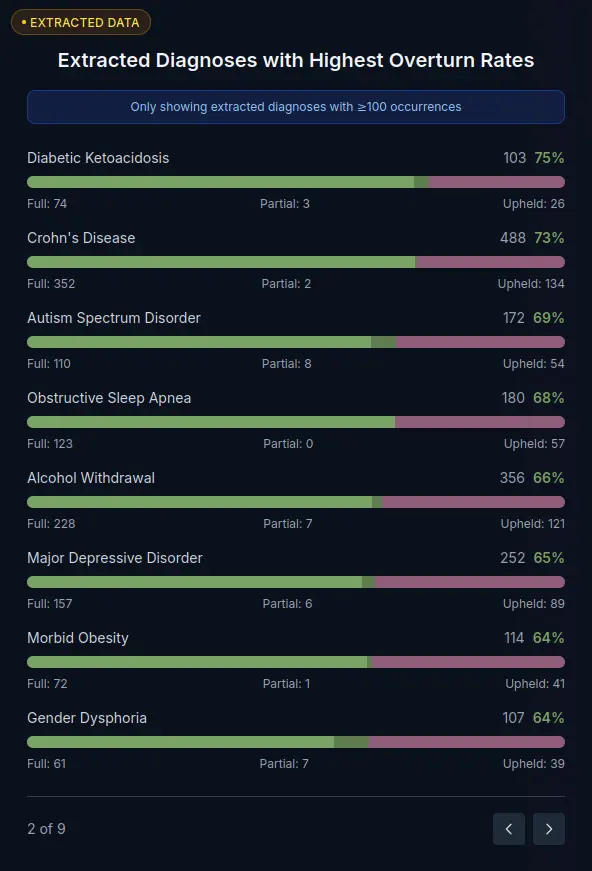
Figure 4. A screenshot showing external appeal overturn rates by specific diagnosis and service categories.
3. Understanding Inappropriate Routing Through Multiple Appeal Levels
We want the ability to understand the extent to which certain types of denial and appeal contexts are being inappropriately routed through multiple levels of appeals at disproportionate rates. Exploring such trends requires making determinations about what it means for denial or appeal contexts to be 'similar'. One approach is requiring they involve the same diagnosis or service, but there are other ways contexts could be similar that could lead to interesting findings (demographic factors, sequences of medical events, etc.).
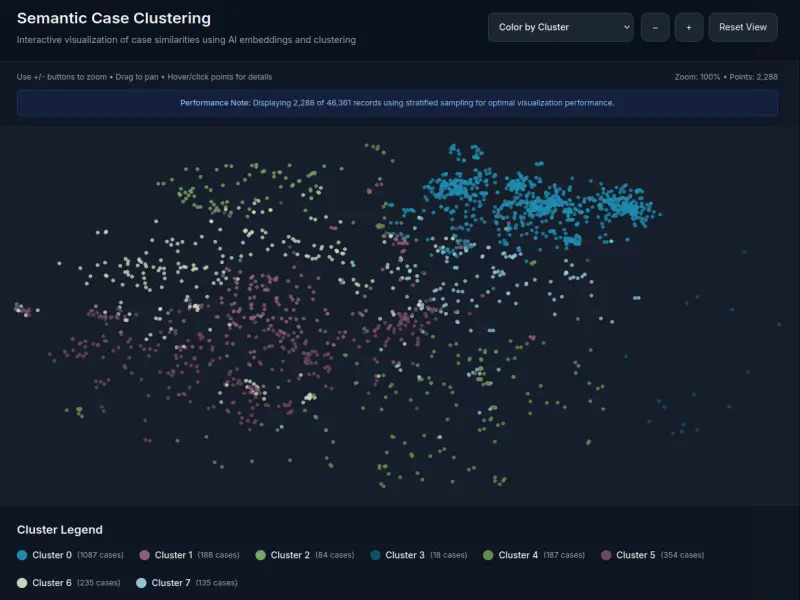
Figure 5. A screenshot showing our approach to clustering cases semantically to investigate trends in outcomes.
What We've Found
Our analysis of the data reveals concerning patterns, which we've been investigating and reporting on for years. External appeal overturn rates vary dramatically by diagnosis and service type, with some of the most vulnerable populations facing the highest rates of inappropriate denials. These findings suggest systemic problems in how certain conditions and treatments are being evaluated by insurers.
The dashboard allows anyone to explore these patterns themselves, filtering by insurer, diagnosis, service type, and other factors to understand where problems are most acute. By measuring, monitoring, and shining light on these trends, we can begin to seek true accountability and measurable improvement.
Support Our Work
This dashboard was built on a volunteer basis, without any funding, to help shine a light on wrongful health insurance denials. If you find it useful, especially in professional work, please consider donating to help us continue building free, accessible technology in the public interest.
Contact
Please direct correspondence with questions, suggestions, or other feedback to info@persius.org.
